The covid-19 pandemic is going to be a rich source of data for how to deal with any future pandemics. The prevalence and degree of severity of the disease has varied widely across the globe, as have the ways in which various countries responded to it, and this has given rise to so-called ‘natural experiments’, those in which one can isolate and study the effects of individual factors without having to actually do experiments.
One of the firmest lessons is the importance of vaccinations for everyone but especially the need to vaccinate those segments of the population that are most likely to suffer adverse effects and death. In the case of covid-19, it was the elderly and the immunocompromised who were most at risk.
But there is also the question of how far to go with trying to isolate regions in order to keep the virus out of the country. The countries that practiced severe lockdowns and strict border controls (such as China, New Zealand, and Hong Kong) were initially able to keep the numbers extremely low while many other countries were suffering badly, but now the situation seems to be reversed in that the previously affected countries are seeing a decline while those initially low case number countries are seeing a spike.
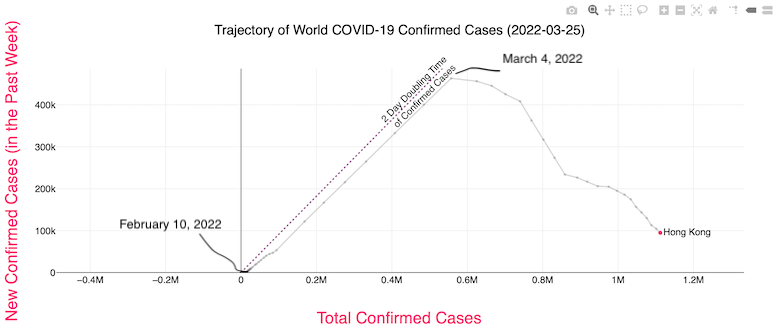
Hong Kong is a particularly interesting case study about the so-called Zero-Covid strategy. Back in January, I described the strict protocols the country had imposed. But recently, things have gone sour. I wrote about the sudden rapid rise in death rates this month in a post last week and in this graph of the number of confirmed cases. We see that it was close to zero until February 10th, shot up to a weekly number of 460,000 by March 4th and then started to decline to the present value of 95,000 per week, compared to about 220,000 per week for the US. Given that the US has a population nearly 50 times that of Kong Kong’s 7.5 million, the Hong Kong per capita rate is huge. The March 4th weekly infections rate would translate to over 20 million in the US. It currently has one of the highest per capita death rates in the world, about three times higher than the highest death rate in the US during the pandemic.
So what happened? Dhruv Khullar spoke to Siddharth Sridhar, a virologist in Hong Kong who described how the medical system was suddenly massively overwhelmed by the sheer numbers and tried to make sense of what has happened. It turned out that part of the problem is a high degree of vaccine skepticism and low vaccination rates, especially among the elderly.
What went wrong? As with surges in many countries, the contributors are numerous and complex. But a key driver appears to be low immunization rates among the elderly. Before the Omicron surge, less than a quarter of people over the age of eighty had been given two doses of a covid vaccine. Meanwhile, the success of Hong Kong’s Zero covid policy meant that few people had acquired natural immunity. In the face of a highly infectious variant, this combination proved combustible, and an under-resourced public health-care system couldn’t extinguish the viral inferno.
Sridhar picked up the narrative.
Locally, the only sign you could see of Zero covid was that everyone was wearing masks. People in Hong Kong had no problem wearing masks. It’s something that was adopted spontaneously in early 2020. You’d see people wearing surgical masks everywhere. I’m talking nearly one-hundred-per-cent compliance. But apart from that, it was very much life as normal. Restaurants were full. Shopping malls were full. People were gathering. There were some nominal restrictions on the number of people who could gather, but, really, it was almost indistinguishable from life before the pandemic.
In general, people viewed covid as something foreign. Like it was something that happened in other parts of the world, but not here. There was almost this condescending attitude about it-that covid was somehow self-inflicted, because people in other places didn’t wear masks enough, or weren’t very attentive to hand hygiene. It was very much, ‘Oh, dear, it’s a problem somewhere else, too bad for them, but this is something that’s preventable.’ That attitude was born because we’d suppressed previous waves so well. In people’s minds, a lot of that was attributable to mask compliance. They felt that if Hong Kong could do it, despite being such a crowded city, why were variants like Delta or Omicron such a problem in other parts of the world?
…Stigma is a real thing when it comes to covid in Hong Kong. If you test positive, it’s terrifying. You get sent off to isolation. Your family is quarantined. If your kids test positive, there’s a separation issue. Even when you come back, you might find that employers aren’t too happy about what happened. Your neighbors tend to shun you.
…In Hong Kong, the perception of covid is that it’s a fatal illness for which you need to seek medical attention irrespective of your disease severity. It isn’t normalized in any way. People are terrified of it. They basically see it as the new SARS. On top of that, the culture here is to go to the emergency department for colds. It’s a big part of the health-seeking culture here. We don’t have a super robust public primary-care system. And the private doctors are very … Let’s just say, there’s a lot of variation in terms of whether they will care for people with covid. The only recourse is to go to the emergency department. So people with any and all severity of covid showed up at emergency departments and flooded the system. It’s a pretty fragile system to begin with. The public health-care infrastructure in Hong Kong is under chronic stress. If you have huge droves of patients coming in, it really hurts.
Media sensationalization added to the problem.
The vaccination problem is especially troubling. In Hong Kong, vaccines are perceived as inherently harmful for older people with chronic medical conditions. It’s been a misconception that we haven’t been able to shake. Once the vaccination campaign took off, you had breathless, wall-to-wall coverage in the media about adverse events in the fourteen days after vaccination. Say a seventy- or eighty-year-old person with cardiovascular risk factors developed a stroke a week after vaccination-it would be a headline. You would find a line somewhere in the article saying that doctors couldn’t find a connection between the vaccine and the event—but who reads that far? You just look at the headline and it’s, like, Stroke after vaccination! And then you’re, like, Oh, vaccines are dangerous for people with chronic medical conditions.
A lot of people in nursing homes don’t have much agency to make their own medical decisions. It’s a big thing in Asia, in general, that older people tend to devolve personal medical decision-making to their kids. The children would be looking at the headlines and the social-media discussion around the vaccines, and they would simply say, ‘You know what, this is too dangerous for you, you’re a fragile individual, it’s going to hurt you. Let me get it instead.’ We have fabulous vaccination uptake in the younger age groups, but it really fell off in the above-sixties, above-seventies.
“Plus, there was never any covid here, right? No one had known someone with severe covid or who’d died of covid. So people felt, Why risk it?
“Now, we’re living with the result.”
It is clear that masks alone are not enough to combat covid-19 and past successes in Hong Kong using just masks may have lulled the population into thinking that it was. In 2009, I made a brief visit to Hong Kong. This was during the time of the swine flu scare and I was impressed with the precautions being taken at the airport, the hotel, and pretty much everywhere, and the near universal wearing of masks.
We also need better reporting on the science, so that the occasional death or severe illness is put in proper context. People get strokes and heart attacks all the time. When you have mass vaccination campaigns, there are going to be people who get a stroke and die soon after getting the vaccine. That kind of anecdotal story has a powerful emotional weight and requires a determined effort to explain why there may be no cause and effect or, even if there was, why the risk of not getting vaccinated may be much greater than the risk due to the occasional side effect.
What seems to be also important is to have a robust public health system that is tied closely to the medical system, like in Costa Rica.
I am just touching the tip of the iceberg here. I hope that all the painfully-learned lessons learned in dealing with this pandemic are not forgotten once it goes away but are used to drive future public health actions globally.

There were some nominal restrictions on the number of people who could gather, but, really, it was almost indistinguishable from life before the pandemic.
I for one got a very different impression from the reports of how HK authorities used the pandemic restrictions as a primary tool in crushing the pro-democracy movement (curiously unmentioned by these public health analyses).
I do think it was better to have strict restrictions and keep the numbers low at the beginning, when there was no vaccine or treatment. The number of deaths would otherwise have been massive, as seen in the US.
They should have, of course, gone into mass vaccination and public information and education as soon as the vaccines came out. But still, I think that their policies have worked out better than America’s have.
How much of the vaccine hesitancy is due to the ineffective made-in-PRC Sinovac vaccine being one of the only two approved vaccines? Pfizer/BioNTech is approved, but are people being given a choice or not told what they’re being given? Is the puppet regime in Hong Kong dictating who gets which vaccine?
From Bloomberg:
The puppet regime has used the media to promote vaccines, but given people’s mistrust of Carrie Lam and Beijing, mistrust of their message on vaccines is inevitable, even if Lam is telling the truth. It also doesn’t help that Hong Kong has one of the highest population densities in the world, over 7000 per square kilometre.
Why does that graph include negative numbers for the Total Confirmed Cases axis? And why is it titled “Trajectory of World COVID-19…” when only Hong Kong and doubling lines are represented?
Ridana @#4,
The site gives data for all countries but that is cluttered and so I chose just Hong Kong. The default is a log-log graph to accommodate the wide range of numbers but I converted it to linear scale for easier reading. The negative x-axis is just an artifact of their graphing routine. The doubling line is the default. You can change it to see what each country’s slope is like.